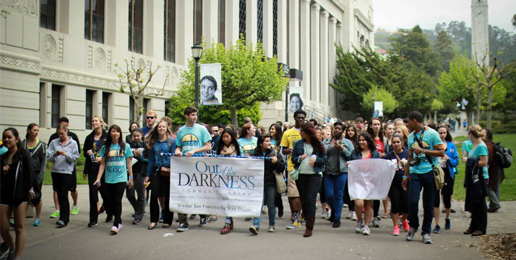
When I was asked by my late daughter Marie’s best friend to join her on a family and friends fundraising walk for suicide prevention last Sunday, I hesitated.
I was in the process of reading yet another disturbing article about assisted suicide, this time a Journal of Clinical Psychiatry article titled “Working with Decisionally Capable Patients Who Are Determined to End Their Own Lives” and I found it outrageous that the suicide prevention groups I know exclude potential physician-assisted suicide victims.
As a nurse, I have personally and professionally cared for many suicidal people over decades including some who were terminally ill. To my knowledge, none of these people went on to die by suicide except one-my own daughter.
Almost nine years ago, my 30 year old daughter Marie died by suicide using an assisted suicide technique she found after searching suicide and assisted suicide websites and reading assisted suicide supporter Derek Humphry’s book “Final Exit”.
Marie was a wonderful woman who achieved a degree in engineering despite struggling off and on with substance abuse and thoughts of suicide for 16 years. She was in an outpatient behavioral health program at the time of her suicide. Her suicide was my worst fear and it devastated all of us in the family as well as her friends. Two people close to Marie also became suicidal after her death but were fortunately saved.
For years before and after Marie’s death, I have written and spoken to groups around the country about the legal and ethical problems with assisted suicide as well as suicide contagion and media reporting guidelines for suicide.
So it was with mixed feelings that I participated in the suicide prevention walk but now I am glad I did.
“WORKING WITH DECISIONALLY CAPABLE PATIENTS WHO ARE DETERMINED TO END THEIR OWN LIVES”
I finally finished reading this article after the walk and found that while the authors of this Journal of Clinical Psychiatry article insist that they are only discussing “decisionally capable” people with “advanced medical illness”, they write:
“The 24% increase in US suicide rates from 1999 to 2014 has led to greater efforts to identify, prevent, and intervene in situations associated with suicidality. While the desire to kill oneself is not synonymous with a mental illness, 80%–90% of completed suicides are associated with a mental disorder, most commonly depression. Understandably, psychiatrists and other clinicians face strong moral, cultural, and professional pressures to do everything possible to avert suicide. Hidden within these statistics are unknown numbers of individuals determined to end their lives, often in the context of a life-limiting physical illness, who have no mental disorder or who, despite having a mental disorder, were nevertheless seemingly rational and decisionally capable and in whom the mental disorder did not seem to influence the desire to hasten death.”
Tragically, the authors also state:
“In reviewing the either sparse or dated literature in this field, surveys from the United States and Canada support that most psychiatrists believe that PAD (physician aid in dying, a euphemism for assisted suicide) should be legal and is ethical in some cases and that they might want the option for themselves.”
And
“Although we see ‘assisted death’ as an option of last resort, we instead ask whether on certain occasions psychiatrists might appropriately not seek to prevent selected decisionally capable individuals from ending their own lives.” (All emphasis added)
This flies in the face of long-standing professional suicide prevention and treatment principles.
Notably, the article ends with an addendum, the 2017 Statement of the American Association of Suicidology (AAS): “Suicide is not the same as ‘Physician Aid in Dying’”
That concludes:
“In general, suicide and physician aid in dying are conceptually, medically, and legally different phenomena, with an undetermined amount of overlap between these two categories” but “Such deaths should not be considered to be cases of suicide and are therefore a matter outside the central focus of the AAS.” (Emphasis added)
WHY I AM GLAD I WENT ON THE SUICIDE PREVENTION WALK
The Sunday walk was sponsored by the American Foundation for Suicide Prevention (AFSP), a group that I discovered states it is trying to “Develop an updated AFSP policy position on assisted death (other common terms include physician assisted suicide or Death with Dignity Laws)”
The next day, I was able to contact a policy person at their Washington, D.C. office and, unlike other suicide prevention group representatives I have contacted in the past, I found this woman surprisingly interested and receptive to the idea that we should not discriminate against certain people when it comes to suicide prevention and treatment. She even asked for my contact information.
Of course, the AFSP may decide to exclude potential assisted suicide victims like other organizations have done but at least I tried and that’s the best tribute I can give to my daughter now.
This article was originally published at NancyValko.com



















